3 results
Hyperoxia in depression
- R. Belmaker, Y. Bloch, P. Shvartzman, P. Romem, Y. Bersudsky, A. Azab
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S688-S689
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies of normobaric hyperoxia in some neurological conditions have demonstrated clinical benefits. Oxygen enriched air may increase oxygen pressure in brain tissue and have biochemical effects such as on brain erythropoietin gene expression, even in patients without lung disease.
ObjectivesThis pilot, randomized, double-blind study examined the efficacy of normobaric hyperoxia as a treatment for depression.
MethodsFifty-five consenting patients aged 18-65 years with mild to moderate depression were included in the study. Participants underwent a psychiatric inclusion assessment and a clinical evaluation by a psychiatric nurse at baseline, 2 and 4 weeks after commencement of study intervention. Participants were randomly assigned to normobaric hyperoxia of 35% fraction of inspired oxygen or 21% fraction of inspired oxygen (room air), through a nasal tube, for 4 weeks, during the night. Patients were rated blindly using the Hamilton Rating Scale for Depression (HRSD); Clinical Global Impression (CGI) questionnaire; Sheehan Disability Scale (SDS).
ResultsThe present study showed a significant improvement in HRSD (p<0.0001), CGI (p<0.01) and in SDS (p<0.05) among patients with depression who were treated with oxygen-enriched air, as compared to patients who were treated with room air. In CGI, 69% of the patients who were treated with oxygen-enriched air improved compared to 23% patients who were treated with room air.
ConclusionsThis small pilot study showed a beneficial effect of normobaric hyperoxia on some symptoms of depression.
DisclosureNo significant relationships.
Schizophrenia in Bilingual Immigrants: is Verbal Fluency Preserved in Second Language Acquisition?
- D. Smirnova, J. Walters, J. Fine, Y. Muchnik-Rozanov, M. Paz, V. Lerner, H. Belmaker, Y. Bersudsky
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Objectives
Language disturbances are the core symptoms of schizophrenia [Crow,2000]. Considering the influence of migration on the symptoms of schizophrenia [Bhugra, Gupta,2011] and few studies on the interaction of schizophrenia and bilingualism [Bersudsky, et al.,2005], we hope to clarify the linguistic profile of disorder and emphasize the role of language in schizophrenia research.
AimTo examine the linguistic features of schizophrenia in the first (L1) and the second (L2) languages, particularly in fluency as the ability to cope with native and nonnative pragmatics.
MethodsAmong sixty Russian immigrants to Israel diagnosed with schizophrenia, ten Russian-Hebrew fluent bilinguals met criteria for inclusion in the study (age: M=33.8,s.d.=11.0; length of residence: M=14.6,s.d.=6.8; time of immigration to diagnosis:M=5.3,s.d=3.9; PANSS Total score: M = 94.9,s.d = 9.8). Interviews were analyzed using clinical, linguistic and fluency speech markers. Statistical evaluation included t-test for dependent samples, two-way ANOVA(Fisher LSD post-hoc test).
ResultsThe mean length of language samples demonstrated more productivity in L1 (Table1). Clinical speech markers associated with thought disorders were similarly represented in both languages. Linguistic markers of schizophrenia occurred more often in L2. Discourse markers, as bilingual phenomenona, reflected more dysfluency in L1.
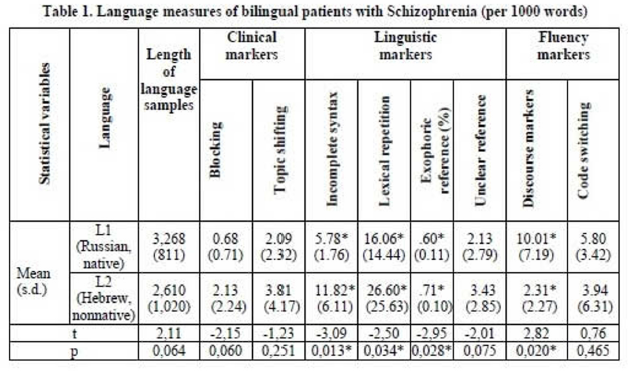 Conclusions
Conclusions1) The higher frequency of linguistic schizophrenia markers in L2 shows more impairments in the syntax/semantic components of language, where different neural representations may underlay the two languages in a bilingual brain damaged by schizophrenia. 2) The higher frequency of fluency markers in L1 reflects attempts to maintain verbal fluency, evidenced by the use of L2 lexical items, which afford a compensatory resource for communicative discourse in schizophrenia.
Influence of birth cohort on age of onset cluster analysis in bipolar I disorder
- M. Bauer, T. Glenn, M. Alda, O.A. Andreassen, E. Angelopoulos, R. Ardau, C. Baethge, R. Bauer, F. Bellivier, R.H. Belmaker, M. Berk, T.D. Bjella, L. Bossini, Y. Bersudsky, E.Y.W. Cheung, J. Conell, M. Del Zompo, S. Dodd, B. Etain, A. Fagiolini, M.A. Frye, K.N. Fountoulakis, J. Garneau-Fournier, A. Gonzalez-Pinto, H. Harima, S. Hassel, C. Henry, A. Iacovides, E.T. Isometsä, F. Kapczinski, S. Kliwicki, B. König, R. Krogh, M. Kunz, B. Lafer, E.R. Larsen, U. Lewitzka, C. Lopez-Jaramillo, G. MacQueen, M. Manchia, W. Marsh, M. Martinez-Cengotitabengoa, I. Melle, S. Monteith, G. Morken, R. Munoz, F.G. Nery, C. O’Donovan, Y. Osher, A. Pfennig, D. Quiroz, R. Ramesar, N. Rasgon, A. Reif, P. Ritter, J.K. Rybakowski, K. Sagduyu, A.M. Scippa, E. Severus, C. Simhandl, D.J. Stein, S. Strejilevich, A. Hatim Sulaiman, K. Suominen, H. Tagata, Y. Tatebayashi, C. Torrent, E. Vieta, B. Viswanath, M.J. Wanchoo, M. Zetin, P.C. Whybrow
-
- Journal:
- European Psychiatry / Volume 30 / Issue 1 / January 2015
- Published online by Cambridge University Press:
- 15 April 2020, pp. 99-105
-
- Article
- Export citation
-
Purpose:
Two common approaches to identify subgroups of patients with bipolar disorder are clustering methodology (mixture analysis) based on the age of onset, and a birth cohort analysis. This study investigates if a birth cohort effect will influence the results of clustering on the age of onset, using a large, international database.
Methods:The database includes 4037 patients with a diagnosis of bipolar I disorder, previously collected at 36 collection sites in 23 countries. Generalized estimating equations (GEE) were used to adjust the data for country median age, and in some models, birth cohort. Model-based clustering (mixture analysis) was then performed on the age of onset data using the residuals. Clinical variables in subgroups were compared.
Results:There was a strong birth cohort effect. Without adjusting for the birth cohort, three subgroups were found by clustering. After adjusting for the birth cohort or when considering only those born after 1959, two subgroups were found. With results of either two or three subgroups, the youngest subgroup was more likely to have a family history of mood disorders and a first episode with depressed polarity. However, without adjusting for birth cohort (three subgroups), family history and polarity of the first episode could not be distinguished between the middle and oldest subgroups.
Conclusion:These results using international data confirm prior findings using single country data, that there are subgroups of bipolar I disorder based on the age of onset, and that there is a birth cohort effect. Including the birth cohort adjustment altered the number and characteristics of subgroups detected when clustering by age of onset. Further investigation is needed to determine if combining both approaches will identify subgroups that are more useful for research.




